Nutrition in Eating Disorder Treatment
We can help you find peace with food with supportive, structured meal planning that focuses on balance, variety and flexibility.

Weight inclusive eating disorder treatment
Eating Recovery Center recognizes the inherent diversity in human bodies and welcomes people of all body shapes and sizes to our weight-inclusive treatment centers. As we focus on health-promoting behaviors, our goal is to take care of you — a whole person — and to help you make choices that support a full, values-aligned life.
Weight-inclusive care means better care for folks in diverse bodies — and it counters weight stigma, a form of discrimination based on a person’s weight or size.
"No matter what your symptoms look like, you deserve support in fostering a peaceful relationship with your body, food and movement. There is hope for a full and lasting recovery – your life can be different."
Adee Levinstein, MS, RD, LD, CED-S
Nutrition Manager for Eating Recovery Center

The importance of meal planning in treatment
Meals play a crucial role in eating disorder treatment and are a critical step towards nutritional rehabilitation. In treatment, patients plan meals with their registered dietitians weekly, reviewing and adjusting meals, food preferences and goals, as needed.
Mealtime can be difficult, and you will feel challenged. By approaching food in a more balanced way, you can move towards a full and lasting recovery. Through collaborative meal planning with your treatment team, normalized eating patterns can return.
For those in on-site care in our inpatient and residential programs, you will typically have three meals and three snacks daily with peers. As you progress through treatment, you will start to have meals and snacks off the unit, with family members and during outings. Some sites offer cooking group experiences as well as grocery store tours.
What is nutritional rehabilitation?
Nutritional rehabilitation is the process of healing malnutrition caused by an eating disorder. This process helps you return to an optimal nutritional status by:
Increasing consistency and structure around meals
Appropriately nourishing your mind and body, leading to improved physical and mental well-being
Reducing or eliminating medical complications
If you’ve been restricting your food intake, you could be experiencing symptoms of malnutrition. Malnutrition can affect people of all body weights, shapes and sizes, harming the brain and body.
How does nutritional rehabilitation work?
Nutritional rehabilitation works by resolving most, if not all, of the physical and mental health consequences the eating disorder has caused. There are many benefits to nutritional rehabilitation, including:
Regulating hormones (for people of all genders), including regulating menstrual cycles
Improving bone health
Increasing energy
Stabilizing moods and reducing depression, anxiety and irritability
Resolving malnutrition
Nutritional rehabilitation is overseen by experienced psychiatrists, registered dietitians, therapists, primary care physicians and nurses who collaborate daily on-site to provide you with the highest quality nutritional care.
"Food is our patients’ number one medication. Without appropriate nutrition, patients’ brains and bodies cannot heal from the devastation of the eating disorder. When food intake does not meet their body’s needs, they won’t get better. Adequate nutrition is vital to recovery; we provide that here."
Jennifer Lewis, RD, LD, CEDRD-S
Nutrition Director, Eating Recovery Center
Selecting meals in treatment
Patients receive support in planning their meals for the week, including breakfast, lunch, dinner and snacks. Adults choose their own menus and caregivers plan menus for child and adolescent patients. The treatment team monitors and evaluates each patient’s nutritional status, adjusting meal plans as needed. Exchange-based meal plans offer flexibility, ensuring that nutritional needs are met.
Addressing dietary restrictions and food allergies in treatment
When you arrive for treatment, please discuss any food allergies or dietary needs with your registered dietitian.
We respect and honor individual dietary restrictions and can accommodate Kosher and Halal diets.
Vegetarian options are provided at each meal.
If you have a documented food allergy, our team will ensure that you will not encounter those items during meals or snacks.
Medical doctors, nurses and registered dietitians are all medically trained to provide patients with diabetes and other health conditions the medical and nutritional support they need.
Find ongoing nutrition therapy support with the Recovery Record app
Adult patients are encouraged to use the Recovery Record app in treatment and after discharge. Parents log in and update the app for child and adolescent patients. This app offers many convenient benefits to those in eating disorder recovery and is widely praised throughout the field. With help from the app, you will be able to:
Log meals and snacks
View meal plans
Discover new coping skills and strategies
Receive encouragement from your treatment team
Stay on track in recovery
The Recovery Record app is available for free in your favorite app store.

Meal support in eating disorder treatment
Mealtime in eating disorder treatment can be challenging and anxiety-provoking. Individuals may feel discomfort due to the refeeding process, challenging their eating disorder rules or for other reasons. During mealtimes and snacks, the treatment team works closely with each patient to provide structure and emotional support. Eating disorder behaviors are monitored and addressed. All of our meal rooms are designed to be as pleasant and welcoming as possible.

Nutrition therapy for children and teens
Through our innovative family program, caregivers are empowered to become agents of change for their loved ones, helping them achieve long-term recovery. Our family-based treatment model views caregivers as an essential part of the treatment plan for child and adolescent patients. Caregivers manage certain aspects of each young patient’s meals. The goal is to eventually eliminate eating disorder behaviors.
The following principles serve as a foundation for our behavioral approach to treatment:
Treating symptoms and behaviors
Focusing on what can be done here and now to support recovery
Encouraging caregivers to lead the way
Identifying caregiver support as essential to the recovery process
Supporting caregivers in supporting their loved ones
Our therapists also serve as coaches, guiding families through the treatment process. Caregivers learn how to support their children through behavior coaching and emotion coaching. These strategies can help caregivers strengthen their relationships with their loved ones as they recover from the eating disorder.

Support for Families & Caregivers
We expect a primary caregiver to be involved in treatment with all of our child and adolescent patients. It is essential that at least one caregiver learn the necessary skills to support the patient’s long-term recovery, including preparing a successful home environment. In treatment, we work together to:
Support you as you learn how to help your child
Teach you how to handle challenges and how to cope with potential setbacks
Help you find and attend support groups for caregivers

Family and Caregiver Support Offerings
Family therapy sessions
Family events
Support groups for caregivers


Nutritional counseling and education
Nutritional counseling and education groups are a fundamental part of eating disorder treatment. During these sessions, you will receive professional and peer support and nutrition education on a variety of topics, along with:
Support with meal and menu planning
Encouragement to process challenging thoughts, feelings and experiences that come up during meals
Values work — learning how to align your behavior with your values
Families and caregivers are also encouraged to attend nutrition education and support groups designed to teach them how to support their loved ones.
Come as you are and find the healing you deserve
Patients come to us with a variety of backgrounds, behaviors and beliefs. Our goal is to provide nutritional rehabilitation that safely helps them achieve optimal physical and mental health. At times, patients need an extra layer of support.
Co-occurring mental health and medical conditions
Most patients with eating disorders experience co-occurring mental health concerns, therefore:
All patients receive psychological support in the form of individual and group therapy.
All patients in inpatient, residential, and partial hospitalization programs receive psychiatric services as part of their care.
All patients in intensive outpatient programs (virtual and on-site) are encouraged to see their outpatient psychiatrists.
Additionally, our on-site programs are staffed with medical doctors and nurses who continuously monitor patients to reduce the risk of physical health complications. Registered dietitians are medically trained to work with patients dealing with physical health concerns, including:
Celiac disease
Food allergies
Diabetes, and more
Supplements and tube feeding available
Our hope is that patients are able to complete the meals and snacks included in their treatment plan. However, we understand this can be challenging. We provide supplements and tube feeding as a “Plan B” for those who are unable to finish meals and snacks. First, we offer a number of incentives to our patients to help them complete meals and snacks. Then, we refer to established guidelines before making a recommendation for supplements or tube feeding.
Support for severe complications related to eating disorders
Supplements
At times, patients struggle to complete their meal plans and need a little more support as part of their nutritional rehabilitation. Supplements help patients meet their nutritional needs so their brains and bodies can heal.
Tube feeding
In some instances, patients are unable to complete their meal plans and supplements. When this occurs, tube feeding may be recommended. This procedure can be vital and lifesaving. When tube feeding is recommended, our experienced medical and nursing staff provide temporary nutritional supplementation via tubes inserted through the nose.
Why ERC?
We are one of the few eating disorder treatment programs who are able to offer tube feeding on-site in our residential programs. The benefit of this service is that patients can stay with their residential treatment team instead of leaving to go to a separate hospital or location, which can be upsetting and disruptive to treatment.
Refeeding syndrome
Refeeding syndrome is a potentially fatal complication that can occur when patients start to eat after a long period of restriction. Our medical doctors and nurses monitor all patients to reduce the risk of refeeding syndrome with established guidelines that include:
Checking labs and vital signs regularly
Being aware of patients at higher risk for refeeding syndrome
Treating early signs of refeeding syndrome, if necessary
Offering patients and families education about refeeding syndrome

Nutrition therapy in binge eating disorder treatment
Our binge eating disorder treatment program is based on a weight-inclusive approach that incorporates:
Nutrition assessment and education
Body image work
Behavior changes related to food and movement
These interventions can bring positive outcomes to all patients, including:
A greater appreciation for body diversity
Reduced disordered eating patterns
Increased self-compassion
More frequent health-supporting behaviors
Increased inner wisdom related to body cues, and more
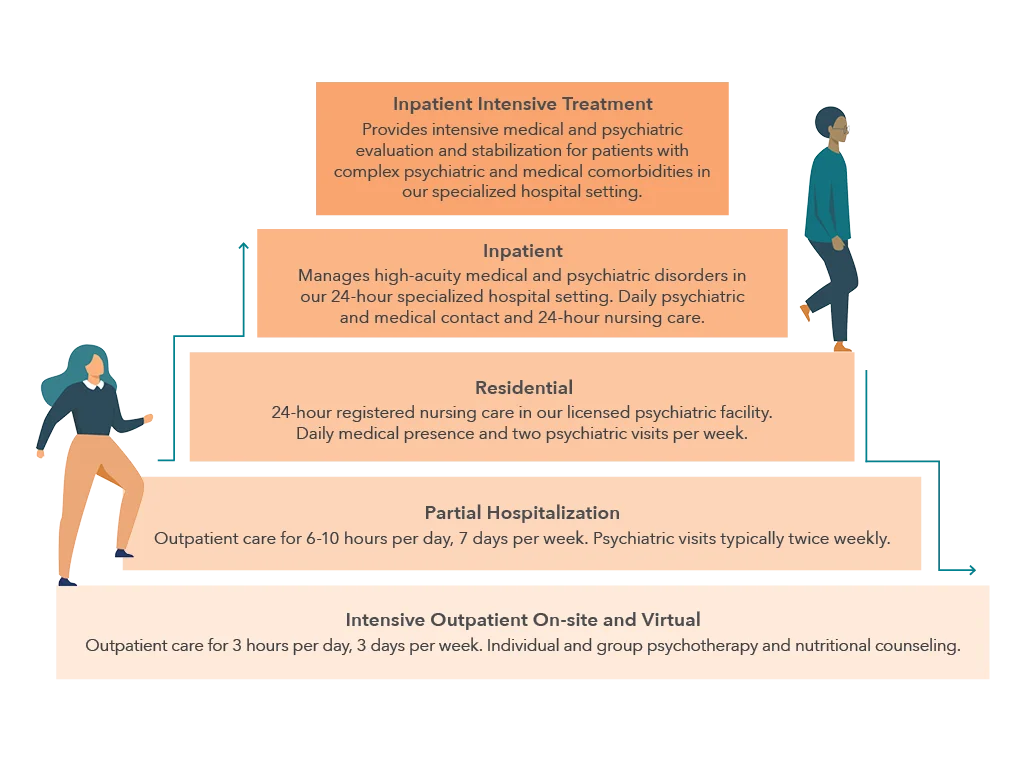
Levels of Care in Eating Disorder Treatment